It’s easier to change your shoe than your foot – that’s the first thing that consultant orthopaedic surgeon Ian Kelly, based at UPMC Whitfield in Waterford, says.
“Surgery is only recommended when other non-surgical treatment has been tried. Whether or not you decide to opt for surgery depends on how the bunion (hallus valgus) deformity is affecting your life.
“If you don’t have much of a problem then you won’t be prepared to give it 12 weeks [to recover]. I always tell patients that it is easier to change your shoe than your foot. You may be able to manage it, but it depends on your symptoms. If you are experiencing terrible pain and you can’t get any footwear to fit you then 12 weeks won’t seem so long,” he says.
He says that bunion surgery isn’t a major operation but it is “significant”.
After the six-week mark, if it looks good, they can start coming out of the stiff post-operative shoe
“The reality is that you are doing the corrections at a bone level (breaking bones) and at a soft tissue level as well so that includes the tendons and ligaments too and it takes at least six weeks for those repairs to heal. What I say to patients is that although it is done as a day-case procedure they will have to use crutches for six weeks with a protective dressing on.
“After the six-week mark, if it looks good, they can start coming out of the stiff post-operative shoe, dressings can be removed and the person can start to weight bear as tolerated, but it does take 12 weeks to get over a bunion operation.”
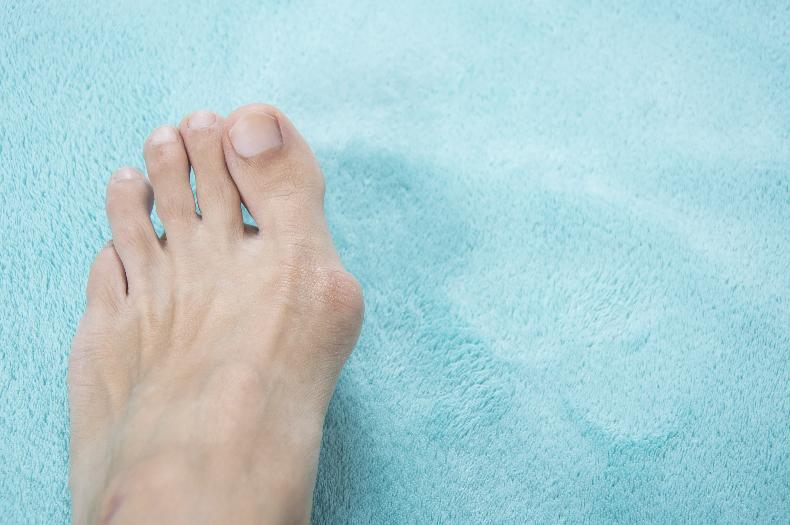
Perhaps contrary to popular opinion, bunions don’t relate to the big toe joint but instead to the soft tissues around the joint.
“The soft tissues on the inner side gets stretched and the soft tissues on the outer side tighten up,” he says, “so when you are correcting a bunion deformity you have to correct both the bone deformity and the soft tissue deformity.”
Second toe pain can result, with inflammation and a “hammer toe” deformity also developing
Hallus is the big toe and valgus describes the direction that the big toe has gone in – that it has drifted across to the second toe.
“Second toe pain can result, with inflammation and a “hammer toe” deformity also developing. There can be friction involved with the second toe also,” he says.
Footwear is main factor
While genetics can be a factor in bunion formation, footwear is thought to be one of the main factors.
“Women tend to wear a shoe with a heel on it, which will drive the forefoot down into what is a narrow toe box. We shouldn’t be wearing narrow fitting shoes with a pointed toe box.
“I often ask the patient to stand on the ground and I outline the natural width and contour of their foot with them standing and then I’ll superimpose their shoe on that drawing. It highlights to patients how they are compressing their foot into their shoe.”
Deep toe boxes needed
People who have a naturally wide forefoot need to be careful about their footwear, he states.
“There’s no problem wearing a fashion shoe to a wedding or on a night out but for the majority of your footwear-wearing time you should be in appropriately fitting, wide-fitting shoes.”
Most podiatrists would know where to source deep toe box shoe
Deep toe boxes are needed for those who have bunions because the second toe sometimes overlaps the big toe and therefore the second toe will friction against the top of the shoe.
“The deep toe box will accommodate the second toe deformity,” he says. “Most podiatrists would know where to source deep toe box shoes and many shoe shops now would have a good range.”
Toe separators – non-surgical solution
If the bunion isn’t causing pain, Mr Kelly recommends consulting a podiatrist/chiropodist and asking him/her to make custom-made toe separators to suit you.
“The ones off the shelf are designed for everybody and fit nobody,” he says, “so you need to have a customised spacer device made for you. If you are in pain because you’re frictioning between the big toe and the second toe then it will stop that problem ie it will address some of the symptoms and at least slow down progression of the deformity.
“Podiatrists have pink Playdoh-like material that they can put between your toes and when ready a few minutes later will exactly accommodate your deformity and fit in comfortably. This will help realign your foot better but bear in mind that it may take one-two months to get used to wearing them.”
Most people don’t need surgery
So when do people make appointments to see a surgeon?
“Some people come because their mother had terrible bunions and they feel that their toes are going in the same direction,” he says.
I never operate unless non-surgical treatment like this has failed
“Some people come because they have a little bit of pain and they are worried about it and some people come at end stage.”
Most of the patients he sees with a bunion deformity don’t need surgery, however.
“I refer many back to a chiropodist and advise them regarding footwear choice. This can mean that they can avoid an operation. I never operate unless non-surgical treatment like this has failed.”
The success rate for the operation is about 90%, he says.
“Most people are very happy they had it done but not everybody, and as with any operation there are risks. That could include infection (very low risk), the deformity recurring (5% risk), the deformity being overcorrected (3% risk) and nerve irritation in the foot (1% risk).”
Teresa Fitzgerald (left) is a dental nurse in Waterford and had bunion surgery in January 2019. 
She has lots of practical advice for anyone considering the operation.
“I would say to people that there are certain things that you need to think about and have in place if you are considering bunion surgery. You can’t drive and you need to have lots of support at home as you will be bedridden for two weeks and wearing a surgical shoe for six. You will need to take three months off work and organise yourself financially also and be a bit mentally prepared as well because you’re going to be confined to your home so much. Having a toilet downstairs in your house would also be very helpful.”
Teresa had noticed the lump on the side of her big toe and over time it began to override her second toe, causing a lump underneath it and pain when she was walking.
“That meant a lot of discomfort for me as a dental nurse on my feet for most of the day so I had to consider surgery. If it had been just the bunion I might have put up with it.”
The surgery itself, done as a day procedure, went very well and the pain medication worked well for her also. She could have done with more tuition about using crutches, however.
“I have a bit of arthritis in my hands so I found them very hard to use. A zimmer frame worked better for me upstairs.”
Upstairs in bed for two weeks Teresa was only allowed to go to the toilet, putting very slight pressure on the heel of the special shoe that she had to wear 24/7. Not having a toilet downstairs after the two weeks caused difficulty for her.
“It meant ‘bumming’ it down the stairs and going up on hands and knees.
“I did have the option of a portable loo downstairs during the day but I didn’t like that option. It was to do with dignity or pride maybe so I made it up and down the stairs but it was very hard.”
For the first few weeks you may not feel great anyway and may not sleep well
Teresa also found that elevating the bed a bit was useful and advised sleeping alone for a couple of weeks if possible.
“That’s to give you space in the bed. For the first few weeks you may not feel great anyway and may not sleep well, so it’s good to have books or a laptop or a TV in the room to occupy yourself so that you can put your mind to something if you wake.”
Because Teresa couldn’t use the crutches well, her daughter rented out a knee scooter for her for six weeks.
“I could pop my leg on it, there is a little basket on the front, you could make tea for yourself, using a cup with a lid. It meant I could move around the house so it gave me a bit of independence. The scooter was great for me but some people mightn’t have the room in their house for it.”
I was probably back to full steam after 12 months
While the medication worked well, Teresa found that she got a lot of jabbing, sharp pain in the toe.
“You’d have to stop and wait until it passed over,” she says. “You would have that for a couple of months and it still happens an odd time when driving and using the clutch.”
Teresa eased back into work gently, doing half days initially.
“I was probably back to full steam after 12 months,” she says, “and it’s so far so good with the operation since.”
Read more
Is the 15-minute COVID-19 test the way of the future?
Healthbytes
It’s easier to change your shoe than your foot – that’s the first thing that consultant orthopaedic surgeon Ian Kelly, based at UPMC Whitfield in Waterford, says.
“Surgery is only recommended when other non-surgical treatment has been tried. Whether or not you decide to opt for surgery depends on how the bunion (hallus valgus) deformity is affecting your life.
“If you don’t have much of a problem then you won’t be prepared to give it 12 weeks [to recover]. I always tell patients that it is easier to change your shoe than your foot. You may be able to manage it, but it depends on your symptoms. If you are experiencing terrible pain and you can’t get any footwear to fit you then 12 weeks won’t seem so long,” he says.
He says that bunion surgery isn’t a major operation but it is “significant”.
After the six-week mark, if it looks good, they can start coming out of the stiff post-operative shoe
“The reality is that you are doing the corrections at a bone level (breaking bones) and at a soft tissue level as well so that includes the tendons and ligaments too and it takes at least six weeks for those repairs to heal. What I say to patients is that although it is done as a day-case procedure they will have to use crutches for six weeks with a protective dressing on.
“After the six-week mark, if it looks good, they can start coming out of the stiff post-operative shoe, dressings can be removed and the person can start to weight bear as tolerated, but it does take 12 weeks to get over a bunion operation.”
Perhaps contrary to popular opinion, bunions don’t relate to the big toe joint but instead to the soft tissues around the joint.
“The soft tissues on the inner side gets stretched and the soft tissues on the outer side tighten up,” he says, “so when you are correcting a bunion deformity you have to correct both the bone deformity and the soft tissue deformity.”
Second toe pain can result, with inflammation and a “hammer toe” deformity also developing
Hallus is the big toe and valgus describes the direction that the big toe has gone in – that it has drifted across to the second toe.
“Second toe pain can result, with inflammation and a “hammer toe” deformity also developing. There can be friction involved with the second toe also,” he says.
Footwear is main factor
While genetics can be a factor in bunion formation, footwear is thought to be one of the main factors.
“Women tend to wear a shoe with a heel on it, which will drive the forefoot down into what is a narrow toe box. We shouldn’t be wearing narrow fitting shoes with a pointed toe box.
“I often ask the patient to stand on the ground and I outline the natural width and contour of their foot with them standing and then I’ll superimpose their shoe on that drawing. It highlights to patients how they are compressing their foot into their shoe.”
Deep toe boxes needed
People who have a naturally wide forefoot need to be careful about their footwear, he states.
“There’s no problem wearing a fashion shoe to a wedding or on a night out but for the majority of your footwear-wearing time you should be in appropriately fitting, wide-fitting shoes.”
Most podiatrists would know where to source deep toe box shoe
Deep toe boxes are needed for those who have bunions because the second toe sometimes overlaps the big toe and therefore the second toe will friction against the top of the shoe.
“The deep toe box will accommodate the second toe deformity,” he says. “Most podiatrists would know where to source deep toe box shoes and many shoe shops now would have a good range.”
Toe separators – non-surgical solution
If the bunion isn’t causing pain, Mr Kelly recommends consulting a podiatrist/chiropodist and asking him/her to make custom-made toe separators to suit you.
“The ones off the shelf are designed for everybody and fit nobody,” he says, “so you need to have a customised spacer device made for you. If you are in pain because you’re frictioning between the big toe and the second toe then it will stop that problem ie it will address some of the symptoms and at least slow down progression of the deformity.
“Podiatrists have pink Playdoh-like material that they can put between your toes and when ready a few minutes later will exactly accommodate your deformity and fit in comfortably. This will help realign your foot better but bear in mind that it may take one-two months to get used to wearing them.”
Most people don’t need surgery
So when do people make appointments to see a surgeon?
“Some people come because their mother had terrible bunions and they feel that their toes are going in the same direction,” he says.
I never operate unless non-surgical treatment like this has failed
“Some people come because they have a little bit of pain and they are worried about it and some people come at end stage.”
Most of the patients he sees with a bunion deformity don’t need surgery, however.
“I refer many back to a chiropodist and advise them regarding footwear choice. This can mean that they can avoid an operation. I never operate unless non-surgical treatment like this has failed.”
The success rate for the operation is about 90%, he says.
“Most people are very happy they had it done but not everybody, and as with any operation there are risks. That could include infection (very low risk), the deformity recurring (5% risk), the deformity being overcorrected (3% risk) and nerve irritation in the foot (1% risk).”
Teresa Fitzgerald (left) is a dental nurse in Waterford and had bunion surgery in January 2019. 
She has lots of practical advice for anyone considering the operation.
“I would say to people that there are certain things that you need to think about and have in place if you are considering bunion surgery. You can’t drive and you need to have lots of support at home as you will be bedridden for two weeks and wearing a surgical shoe for six. You will need to take three months off work and organise yourself financially also and be a bit mentally prepared as well because you’re going to be confined to your home so much. Having a toilet downstairs in your house would also be very helpful.”
Teresa had noticed the lump on the side of her big toe and over time it began to override her second toe, causing a lump underneath it and pain when she was walking.
“That meant a lot of discomfort for me as a dental nurse on my feet for most of the day so I had to consider surgery. If it had been just the bunion I might have put up with it.”
The surgery itself, done as a day procedure, went very well and the pain medication worked well for her also. She could have done with more tuition about using crutches, however.
“I have a bit of arthritis in my hands so I found them very hard to use. A zimmer frame worked better for me upstairs.”
Upstairs in bed for two weeks Teresa was only allowed to go to the toilet, putting very slight pressure on the heel of the special shoe that she had to wear 24/7. Not having a toilet downstairs after the two weeks caused difficulty for her.
“It meant ‘bumming’ it down the stairs and going up on hands and knees.
“I did have the option of a portable loo downstairs during the day but I didn’t like that option. It was to do with dignity or pride maybe so I made it up and down the stairs but it was very hard.”
For the first few weeks you may not feel great anyway and may not sleep well
Teresa also found that elevating the bed a bit was useful and advised sleeping alone for a couple of weeks if possible.
“That’s to give you space in the bed. For the first few weeks you may not feel great anyway and may not sleep well, so it’s good to have books or a laptop or a TV in the room to occupy yourself so that you can put your mind to something if you wake.”
Because Teresa couldn’t use the crutches well, her daughter rented out a knee scooter for her for six weeks.
“I could pop my leg on it, there is a little basket on the front, you could make tea for yourself, using a cup with a lid. It meant I could move around the house so it gave me a bit of independence. The scooter was great for me but some people mightn’t have the room in their house for it.”
I was probably back to full steam after 12 months
While the medication worked well, Teresa found that she got a lot of jabbing, sharp pain in the toe.
“You’d have to stop and wait until it passed over,” she says. “You would have that for a couple of months and it still happens an odd time when driving and using the clutch.”
Teresa eased back into work gently, doing half days initially.
“I was probably back to full steam after 12 months,” she says, “and it’s so far so good with the operation since.”
Read more
Is the 15-minute COVID-19 test the way of the future?
Healthbytes







SHARING OPTIONS